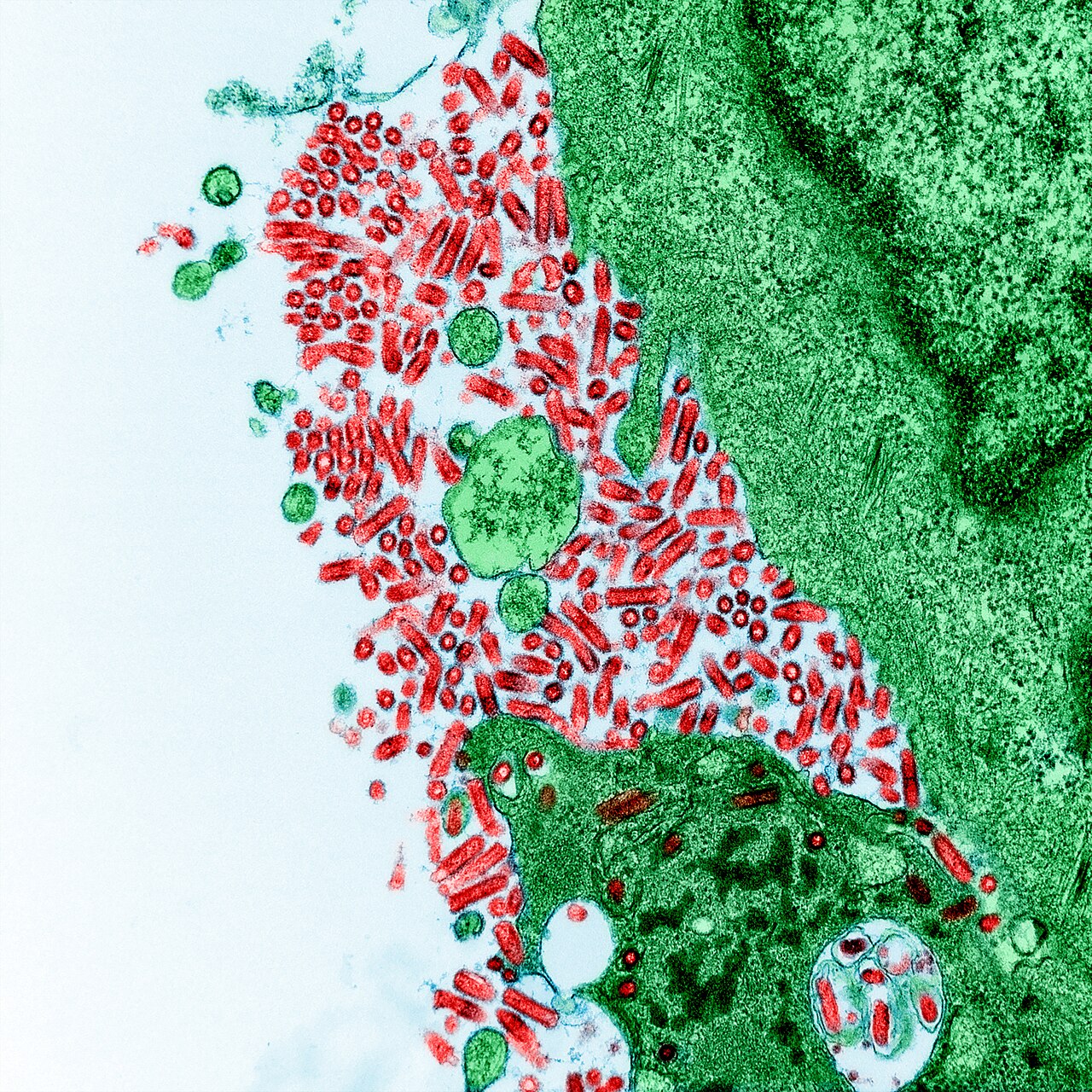
The Rabies Virus: Global Killer, Vaccine Hope, Eradication Goal
The mere mention of the word "rabies" often conjures images of frothing, aggressive animals, a chilling testament to one of humanity's oldest and most feared diseases. Caused by the formidable
Rabies Virus, this zoonotic pathogen remains a significant global health threat, claiming tens of thousands of lives annually, predominantly in vulnerable communities. Yet, amidst its deadly reputation, lies a powerful narrative of scientific triumph: rabies is a vaccine-preventable disease, and global efforts are steadily pushing towards its eradication. Understanding this complex virus, its mechanisms, and the crucial interventions available is key to achieving a world free from its grip.
Unmasking the Rabies Virus: Structure, Function, and Fatal Impact
At its core, the
Rabies Virus (scientifically known as
Rabies lyssavirus) is a marvel of evolutionary engineering, belonging to the genus
Lyssavirus within the family
Rhabdoviridae and order
Mononegavirales. Its distinctive bullet-shaped morphology, an enveloped structure approximately 60 nm in diameter and 180 nm in length, hints at its unique method of cellular invasion. This single-stranded, negative-sense RNA virus is remarkably compact, yet it encodes five essential proteins: nucleoprotein (N), phosphoprotein (P), matrix protein (M), glycoprotein (G), and large polymerase (L). Each of these proteins plays a vital role in the virus's replication cycle, from encapsulating its genetic material to facilitating entry into host cells and suppressing host immune responses.
Once it breaches the mammalian host, the
Rabies Virus initiates an acute, progressive, and almost universally fatal disease. Its primary target is the central nervous system (CNS), leading to a severe inflammatory condition of the brain and spinal cord known as encephalomyelitis. The insidious nature of rabies lies in its delayed onset; clinical symptoms often don't manifest until the virus has extensively damaged the CNS, at which point the disease becomes almost impossible to treat, highlighting the critical importance of early intervention.
Transmission Dynamics: How the Rabies Virus Spreads (and Why Indirect Spread is Rare)
Transmission of the
Rabies Virus occurs primarily through direct contact with infected saliva, typically via the bite or scratch of a rabid animal. When an animal becomes infected, the virus travels to its salivary glands, making its saliva highly infectious. The introduction of this virus-laden saliva into an open wound or mucous membrane provides the pathogen with a direct pathway to a new host.
Globally, domestic dogs are the overwhelming culprits in human rabies cases, accounting for up to 99% of all fatalities. This staggering statistic underscores the pivotal role of canine populations in the epidemiology of the disease, largely due to their close proximity to humans, high population densities in many regions, and sometimes unmanaged roaming behaviors. In contrast, while wildlife such as bats, raccoons, foxes, and skunks serve as significant reservoirs in certain geographic areas (particularly in the Americas), their direct contribution to human cases is comparatively lower than that of dogs.
It's crucial to understand that the
Rabies Virus is remarkably fragile outside a living host, which is why indirect transmission (via fomites or environmental contact) is exceedingly rare. The virus is rapidly inactivated by desiccation (drying in air), sunlight, and even moderate temperatures. For instance, once virus-containing material like saliva dries, it generally loses its infectivity. Survival time outside the host is highly dependent on environmental conditions:
* At room temperature, the virus typically survives no more than a few hours.
* At 30°C with sunlight exposure, inactivation occurs even faster, often within 1.5 hours.
* Studies show survival on surfaces at 20°C can range from 24-48 hours before significant loss of infectivity, with total inactivation usually within a few days.
This inherent fragility means that while caution is always advised, concern over catching rabies from casual contact with surfaces or dried saliva is generally unfounded. For a deeper dive into this aspect, you can explore
Rabies Virus: Structure, Transmission, and Why Indirect Spread is Rare.
The Deadly Journey: From Bite to Brain
Once the
Rabies Virus enters the body, its journey is a precisely orchestrated, albeit deadly, one. It first binds to specific receptors, primarily nicotinic acetylcholine receptors, located on nerve endings near the site of entry. From there, it embarks on a retrograde journey, traveling "backwards" along the peripheral nerves towards the central nervous system. This slow, steady axonal transport allows the virus to largely evade the host's immune surveillance mechanisms in the early stages, making detection before symptoms challenging.
Upon reaching the spinal cord and then the brain, the virus begins to replicate extensively within neurons. This replication causes widespread inflammation, neuronal dysfunction, and ultimately, the characteristic and devastating symptoms of rabies. These can include:
*
Hydrophobia: An intense fear of water, often manifesting as painful spasms of the throat muscles when attempting to drink or even seeing water.
*
Aerophobia: A similar fear triggered by drafts of air.
*
Agitation and hyperactivity: Leading to aggressive behavior, confusion, and hallucinations.
*
Paralysis: Beginning at the bite site and progressing throughout the body.
*
Coma: The final stage before death.
The progression of symptoms from initial discomfort to full-blown encephalomyelitis can vary but is relentlessly progressive. Once these clinical signs become apparent, the disease is almost invariably fatal.
Vaccine Hope and the Global Eradication Goal
Despite the grim prognosis once symptoms appear, the story of the
Rabies Virus is not without hope. Rabies is, remarkably, one of the few deadly diseases that is 100% vaccine-preventable. The development of effective human and animal vaccines dates back to the late 19th century, a monumental achievement in medical history.
Modern prevention strategies involve two key approaches:
1.
Pre-exposure Prophylaxis (PrEP): This involves a series of rabies vaccines administered before potential exposure. It is highly recommended for individuals at elevated risk, such as veterinarians, animal handlers, laboratory workers who deal with the virus, and travelers to regions where rabies is endemic. PrEP simplifies post-exposure treatment and provides a crucial layer of protection.
2.
Post-exposure Prophylaxis (PEP): This is the emergency treatment given *after* suspected exposure to the virus. PEP is a life-saving intervention that must be administered as promptly as possible before the onset of symptoms. It typically comprises three critical steps:
* Immediate and thorough cleansing of the wound with soap and water for at least 15 minutes.
* Administration of rabies immunoglobulin (RIG) into and around the wound, providing immediate passive immunity.
* A series of rabies vaccines over several days, which stimulates the body's own immune system to produce antibodies.
Despite these highly effective interventions, rabies remains a significant public health burden. An estimated 59,000 human deaths occur annually, with over 95% of these fatalities concentrated in Asia and Africa. A particularly tragic statistic is that children under 15 years of age comprise about 40% of victims. This disparity is largely attributable to limited access to PEP in low-resource settings, where poverty, lack of infrastructure, and insufficient healthcare access prevent timely treatment.
Recognizing this critical need, global health organizations like the World Health Organization (WHO) have spearheaded ambitious initiatives. The "Zero by 30" initiative aims to eliminate human deaths from dog-mediated rabies by 2030. This goal is primarily pursued through two powerful strategies:
*
Mass Dog Vaccination: Vaccinating at least 70% of dog populations in endemic areas effectively breaks the chain of transmission from animals to humans. This "one health" approach is not only cost-effective but also protects animal welfare.
*
Improved Surveillance and Access to PEP: Enhancing disease monitoring, strengthening healthcare infrastructure, and ensuring readily available PEP are crucial to managing and preventing human cases.
Practical Insights and Prevention Tips
Empowering individuals with knowledge and actionable advice is paramount in the fight against rabies. Here are essential tips for preventing exposure to the
Rabies Virus:
*
Vaccinate Your Pets: Ensure your dogs, cats, and ferrets are vaccinated against rabies according to local regulations. This is the single most effective way to protect your family and community from domestic animal-mediated rabies.
*
Avoid Wildlife and Stray Animals: Never approach, handle, or feed wild animals (bats, raccoons, foxes, skunks, etc.) or unfamiliar stray dogs and cats, even if they appear friendly. Report any suspicious-acting animals to local animal control authorities.
*
Educate Children: Teach children about the dangers of rabies and the importance of never touching unfamiliar animals.
*
Secure Pet Food and Garbage: Prevent attracting wild animals to your property by keeping pet food indoors and securing garbage cans.
*
Seek Medical Attention Immediately After a Bite: If you or someone you know is bitten or scratched by an animal, especially one suspected of having rabies, immediately wash the wound thoroughly with soap and water for at least 15 minutes. Then, seek urgent medical evaluation for post-exposure prophylaxis. Time is of the essence.
*
Traveler Awareness: If traveling to regions where rabies is endemic, consider pre-exposure vaccination and be aware of the local animal populations. Learn more about effective strategies by reading
Rabies Virus Explained: Transmission, Symptoms, and Prevention Strategies.
Conclusion
The
Rabies Virus represents a dichotomy: a universally fatal disease that is also entirely preventable. Its cunning ability to target the central nervous system and its prevalence in vulnerable populations make it a persistent global health challenge. However, thanks to effective vaccines, both for humans and animals, and dedicated international efforts like the "Zero by 30" initiative, the dream of eradicating human deaths from rabies is within reach. By understanding the virus, promoting responsible pet ownership, practicing vigilance around wildlife, and ensuring access to timely medical intervention, we can collectively work towards a future where the fear of rabies becomes a relic of the past.